-
-
-
Jakarta, Indonesia
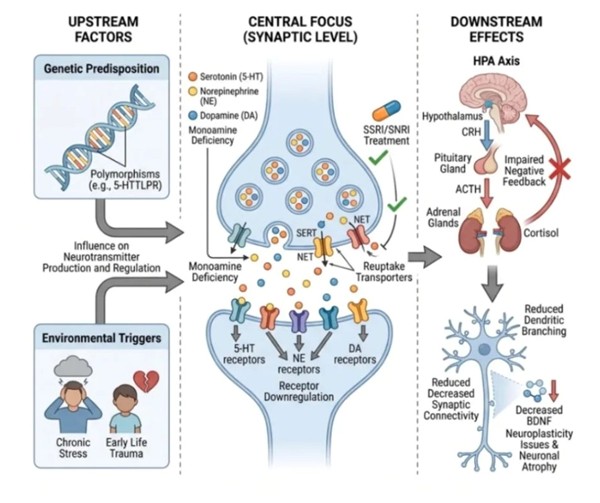
The Silent Atrophy: Why We Are Rewriting Rules on Major Depressive Disorders?

Motion is Lotion: Why the Gym is the Unexpected Best Friend of Your Osteoarthritis
The Couch Is Not the Treatment
There is a deeply human logic to resting a painful joint. When every step produces a dull ache that builds through the day, when stairs become negotiations between the desire to move and the anticipation of pain, when the knee that once carried a person through decades of ordinary life now announces its deterioration with each change in position — the impulse to stop, sit, and protect is not weakness or laziness. It is a biological reflex, a hardwired pain-avoidance behavior that has served the human organism well in the context of acute injury. The problem is that osteoarthritis is not an acute injury. And the couch, for all its apparent comfort, is making it worse.
Osteoarthritis is the most prevalent joint disease in the world and the leading cause of pain-related disability in adults over the age of fifty. It affects an estimated 500 million people globally, with the knee joint bearing the largest share of the burden, followed by the hip and the joints of the hand. Its societal cost — in lost productivity, healthcare utilization, surgical intervention, and the silent erosion of quality of life that accompanies chronic pain — is enormous. And yet the primary therapy for osteoarthritis, supported by more clinical evidence than any drug on the market for this condition, is something that does not require a prescription, a pharmacy, or a surgical suite. It requires a pair of appropriate shoes and the willingness to move.
This article makes the case for exercise as medicine in osteoarthritis — not as a gentle lifestyle supplement to pharmacological management, but as the foundational therapeutic intervention around which all other treatment should be organized. To make that case properly, it is necessary first to understand what osteoarthritis actually is, why the joint behaves as it does, and why the intuition to protect a painful joint through inactivity is not merely unhelpful but actively harmful.
Osteoarthritis is the most prevalent joint disease in the world and the leading cause of pain-related disability in adults over the age of fifty. It affects an estimated 500 million people globally, with the knee joint bearing the largest share of the burden, followed by the hip and the joints of the hand. Its societal cost — in lost productivity, healthcare utilization, surgical intervention, and the silent erosion of quality of life that accompanies chronic pain — is enormous. And yet the primary therapy for osteoarthritis, supported by more clinical evidence than any drug on the market for this condition, is something that does not require a prescription, a pharmacy, or a surgical suite. It requires a pair of appropriate shoes and the willingness to move.
This article makes the case for exercise as medicine in osteoarthritis — not as a gentle lifestyle supplement to pharmacological management, but as the foundational therapeutic intervention around which all other treatment should be organized. To make that case properly, it is necessary first to understand what osteoarthritis actually is, why the joint behaves as it does, and why the intuition to protect a painful joint through inactivity is not merely unhelpful but actively harmful.
What Osteoarthritis Actually Is — and What It Is Not
The dominant cultural conception of osteoarthritis — the one that lives in the minds of most patients and, unfortunately, many of their clinicians — is of a wear-and-tear disease: a passive, mechanical wearing down of joint cartilage that proceeds inevitably with age, like the thinning of a car tire after too many miles. This conception is not entirely wrong, but it is profoundly incomplete, and the incompleteness matters clinically because it produces the therapeutic nihilism — the sense that nothing meaningful can be done beyond pain management and eventual joint replacement — that leaves millions of patients under-treated and overmedicated.
Osteoarthritis is better understood as a failure of joint homeostasis — a condition in which the normal equilibrium between cartilage matrix synthesis and degradation, between load-bearing and biological repair, between inflammatory and anti-inflammatory signaling, has been disrupted beyond the joint's capacity to self-correct. Articular cartilage, the smooth, avascular, aneural tissue that lines the bony surfaces of synovial joints and enables their frictionless gliding motion, is not a passive structural material. It is a biologically active tissue whose chondrocytes continuously synthesize and remodel the collagen and proteoglycan matrix in response to mechanical loading signals.
In early osteoarthritis, this homeostatic balance tips toward degradation: matrix metalloproteinases and aggrecanases — enzymes upregulated by inflammatory cytokines including interleukin-1-beta and TNF-alpha — outpace the synthetic capacity of chondrocytes, producing progressive loss of cartilage thickness, surface fibrillation, and the loss of the viscoelastic properties that make healthy cartilage an extraordinary load-distributing material. As cartilage thins, the subchondral bone beneath it undergoes remodeling — sclerosis, cyst formation, and the development of osteophytes at the joint margins — and the synovial lining becomes chronically inflamed, producing the low-grade synovitis that contributes substantially to the pain experience of osteoarthritis.
Critically, osteoarthritis is not an end-stage process in which cartilage has already been completely destroyed and nothing biological remains to be influenced. In its early and moderate stages, the disease involves active biological processes — inflammatory signaling, chondrocyte metabolic activity, synovial fluid composition, and muscular load-sharing — all of which are meaningfully modifiable by physical exercise. The joint is not a dead structure. It is a living one, capable of responding to the right inputs — and physical loading is among the most potent biological inputs a joint can receive.
Osteoarthritis is better understood as a failure of joint homeostasis — a condition in which the normal equilibrium between cartilage matrix synthesis and degradation, between load-bearing and biological repair, between inflammatory and anti-inflammatory signaling, has been disrupted beyond the joint's capacity to self-correct. Articular cartilage, the smooth, avascular, aneural tissue that lines the bony surfaces of synovial joints and enables their frictionless gliding motion, is not a passive structural material. It is a biologically active tissue whose chondrocytes continuously synthesize and remodel the collagen and proteoglycan matrix in response to mechanical loading signals.
In early osteoarthritis, this homeostatic balance tips toward degradation: matrix metalloproteinases and aggrecanases — enzymes upregulated by inflammatory cytokines including interleukin-1-beta and TNF-alpha — outpace the synthetic capacity of chondrocytes, producing progressive loss of cartilage thickness, surface fibrillation, and the loss of the viscoelastic properties that make healthy cartilage an extraordinary load-distributing material. As cartilage thins, the subchondral bone beneath it undergoes remodeling — sclerosis, cyst formation, and the development of osteophytes at the joint margins — and the synovial lining becomes chronically inflamed, producing the low-grade synovitis that contributes substantially to the pain experience of osteoarthritis.
Critically, osteoarthritis is not an end-stage process in which cartilage has already been completely destroyed and nothing biological remains to be influenced. In its early and moderate stages, the disease involves active biological processes — inflammatory signaling, chondrocyte metabolic activity, synovial fluid composition, and muscular load-sharing — all of which are meaningfully modifiable by physical exercise. The joint is not a dead structure. It is a living one, capable of responding to the right inputs — and physical loading is among the most potent biological inputs a joint can receive.
Motion is Lotion: The Biology of Why Movement Heals Synovial Fluid: The Joint's Internal Pharmacy
The phrase "motion is lotion" is a mnemonic, not a metaphor — it describes a precise biological mechanism. Articular cartilage is avascular: it has no blood supply, and it therefore cannot receive nutrients through the vascular delivery system that sustains every other tissue in the body. Instead, it depends entirely on diffusion from the synovial fluid that bathes the joint cavity for its oxygen, glucose, growth factors, and the metabolic substrates that its chondrocytes require to maintain matrix synthesis. This diffusion is not passive — it is driven by the mechanical compression and relaxation cycle of joint loading.
When a joint is loaded — when a person walks, cycles, swims, or performs any exercise that moves the articular surfaces — the cartilage is cyclically compressed and decompressed. During compression, fluid is expressed from the cartilage matrix into the joint cavity; during decompression, nutrient-rich synovial fluid is drawn back in. This pumping mechanism is the primary means by which chondrocytes receive their nutritional supply and by which metabolic waste products are cleared from the cartilage matrix. A joint that is not moved is a joint whose cartilage is nutritionally deprived — and nutritionally deprived chondrocytes downregulate matrix synthesis while upregulating degradative enzyme production, accelerating precisely the homeostatic imbalance that defines osteoarthritis.
Beyond the nutritional pump, physical activity influences synovial fluid composition in ways that are directly beneficial to joint health. Exercise increases the synovial membrane's production of hyaluronic acid — the high-molecular-weight glycosaminoglycan that is the primary determinant of synovial fluid viscosity and its lubricating properties. In osteoarthritic joints, hyaluronic acid concentration and molecular weight are reduced, contributing to the increased friction, reduced shock-absorption, and impaired joint lubrication that exacerbate both pain and cartilage wear. Physical activity, by stimulating synoviocyte hyaluronic acid synthesis, partially reverses this deficit and restores something closer to the joint's native lubricating environment.
When a joint is loaded — when a person walks, cycles, swims, or performs any exercise that moves the articular surfaces — the cartilage is cyclically compressed and decompressed. During compression, fluid is expressed from the cartilage matrix into the joint cavity; during decompression, nutrient-rich synovial fluid is drawn back in. This pumping mechanism is the primary means by which chondrocytes receive their nutritional supply and by which metabolic waste products are cleared from the cartilage matrix. A joint that is not moved is a joint whose cartilage is nutritionally deprived — and nutritionally deprived chondrocytes downregulate matrix synthesis while upregulating degradative enzyme production, accelerating precisely the homeostatic imbalance that defines osteoarthritis.
Beyond the nutritional pump, physical activity influences synovial fluid composition in ways that are directly beneficial to joint health. Exercise increases the synovial membrane's production of hyaluronic acid — the high-molecular-weight glycosaminoglycan that is the primary determinant of synovial fluid viscosity and its lubricating properties. In osteoarthritic joints, hyaluronic acid concentration and molecular weight are reduced, contributing to the increased friction, reduced shock-absorption, and impaired joint lubrication that exacerbate both pain and cartilage wear. Physical activity, by stimulating synoviocyte hyaluronic acid synthesis, partially reverses this deficit and restores something closer to the joint's native lubricating environment.
Mechanical Loading and Chondroprotection
The relationship between mechanical loading and cartilage biology is not simply that movement is better than rest — it is that the appropriate level and type of mechanical loading is actively chondroprotective, promoting chondrocyte anabolism and suppressing the catabolic signaling pathways that drive cartilage degradation. Chondrocytes are mechanosensitive cells: they express mechanoreceptors including integrins, ion channels, and primary cilia that transduce physical compression into intracellular biochemical signals, and the nature of those signals — anabolic or catabolic — depends critically on the magnitude and frequency of the loading stimulus.
Moderate, cyclic loading — the loading pattern produced by walking, cycling, swimming, and resistance exercise — activates anabolic signaling pathways in chondrocytes, promoting the synthesis of collagen type II and aggrecan, the principal structural components of the articular cartilage matrix, while suppressing the production of matrix metalloproteinases and inflammatory cytokines. High-impact, repetitive loading — such as that produced by running on hard surfaces without adequate muscular support, or by contact sports in patients with existing significant cartilage loss — can exceed the chondroprotective threshold and tip the balance toward catabolism. This distinction is clinically important: it means that exercise prescription for osteoarthritis requires individualization, not blanket restriction, and that the goal is to identify the loading modality that provides chondroprotective mechanical stimulation without exceeding the joint's load-bearing capacity.
Moderate, cyclic loading — the loading pattern produced by walking, cycling, swimming, and resistance exercise — activates anabolic signaling pathways in chondrocytes, promoting the synthesis of collagen type II and aggrecan, the principal structural components of the articular cartilage matrix, while suppressing the production of matrix metalloproteinases and inflammatory cytokines. High-impact, repetitive loading — such as that produced by running on hard surfaces without adequate muscular support, or by contact sports in patients with existing significant cartilage loss — can exceed the chondroprotective threshold and tip the balance toward catabolism. This distinction is clinically important: it means that exercise prescription for osteoarthritis requires individualization, not blanket restriction, and that the goal is to identify the loading modality that provides chondroprotective mechanical stimulation without exceeding the joint's load-bearing capacity.
The Gym as Medicine: Muscles as Biological Shock Absorbers
The most mechanistically direct argument for exercise in osteoarthritis is the role of periarticular muscle as a biological shock absorber. The knee joint, to take the most clinically prevalent example, does not bear load in isolation. Every step transmits ground reaction forces that are many times body weight through the lower limb, and the distribution of those forces between the articular cartilage and the soft tissue structures surrounding the joint — including the quadriceps, hamstrings, calf musculature, and the joint capsule and ligamentous structures — is determined largely by the strength, timing, and coordination of the periarticular muscles.
In patients with knee osteoarthritis, quadriceps weakness is among the most consistent and clinically significant findings on physical examination. Studies using dynamometric assessment consistently demonstrate that quadriceps strength is reduced by twenty to thirty percent in patients with knee osteoarthritis compared to age-matched controls — a deficit that appears to precede radiographic evidence of joint damage in some patients and that correlates more strongly with pain severity and functional limitation than does the degree of cartilage loss on imaging. The quadriceps weakness of osteoarthritis is not merely a consequence of pain-related disuse atrophy; it reflects, in part, neurological inhibition of quadriceps motor unit recruitment driven by afferent signaling from the inflamed synovial joint — a phenomenon termed arthrogenic muscle inhibition that persists even when pain is acutely managed.
The therapeutic consequence of this understanding is clear and actionable: strengthening the quadriceps reduces the dynamic load transmitted through the medial tibiofemoral compartment — the most commonly affected compartment in knee osteoarthritis — by improving the neuromuscular control of joint loading during functional activities. A quadriceps muscle that contracts with appropriate force and timing during the loading response phase of gait acts as an energy-absorbing spring, dissipating a portion of the impact load before it reaches the articular surfaces. A weak, inhibited quadriceps transfers that load directly to cartilage, meniscus, and subchondral bone, accelerating the structural damage that drives further pain and further weakness in the vicious cycle that characterizes progressive knee osteoarthritis.
Resistance training — structured, progressive loading of the quadriceps, hamstrings, hip abductors, and calf musculature — is therefore not merely a fitness intervention for patients with osteoarthritis. It is a biomechanical intervention that directly modifies the stress environment of the articular cartilage, reduces the mechanical drivers of cartilage degradation, and restores the neuromuscular architecture that the joint's own inflammatory signaling has progressively dismantled. The gym is not where osteoarthritis patients go when they have exhausted other options. It is where they should go first.
In patients with knee osteoarthritis, quadriceps weakness is among the most consistent and clinically significant findings on physical examination. Studies using dynamometric assessment consistently demonstrate that quadriceps strength is reduced by twenty to thirty percent in patients with knee osteoarthritis compared to age-matched controls — a deficit that appears to precede radiographic evidence of joint damage in some patients and that correlates more strongly with pain severity and functional limitation than does the degree of cartilage loss on imaging. The quadriceps weakness of osteoarthritis is not merely a consequence of pain-related disuse atrophy; it reflects, in part, neurological inhibition of quadriceps motor unit recruitment driven by afferent signaling from the inflamed synovial joint — a phenomenon termed arthrogenic muscle inhibition that persists even when pain is acutely managed.
The therapeutic consequence of this understanding is clear and actionable: strengthening the quadriceps reduces the dynamic load transmitted through the medial tibiofemoral compartment — the most commonly affected compartment in knee osteoarthritis — by improving the neuromuscular control of joint loading during functional activities. A quadriceps muscle that contracts with appropriate force and timing during the loading response phase of gait acts as an energy-absorbing spring, dissipating a portion of the impact load before it reaches the articular surfaces. A weak, inhibited quadriceps transfers that load directly to cartilage, meniscus, and subchondral bone, accelerating the structural damage that drives further pain and further weakness in the vicious cycle that characterizes progressive knee osteoarthritis.
Resistance training — structured, progressive loading of the quadriceps, hamstrings, hip abductors, and calf musculature — is therefore not merely a fitness intervention for patients with osteoarthritis. It is a biomechanical intervention that directly modifies the stress environment of the articular cartilage, reduces the mechanical drivers of cartilage degradation, and restores the neuromuscular architecture that the joint's own inflammatory signaling has progressively dismantled. The gym is not where osteoarthritis patients go when they have exhausted other options. It is where they should go first.
The Evidence: What Clinical Trials Tell Us About Exercise and Osteoarthritis
The evidence base for exercise in osteoarthritis is not merely suggestive — it is, by the standards of musculoskeletal medicine, exceptionally strong. Multiple systematic reviews and meta-analyses, including those commissioned by the Osteoarthritis Research Society International, the European League Against Rheumatism, and the American College of Rheumatology, have consistently identified exercise as one of the few interventions in osteoarthritis management with both high-quality evidence and a favorable benefit-to-risk profile. All major international guidelines for knee and hip osteoarthritis management now list exercise as a core, first-line recommendation — a status that no currently available pharmacological therapy for osteoarthritis enjoys.
The ESCAPE-pain program — Enabling Self-management and Coping of Arthritic Pain through Exercise — a structured group rehabilitation program developed in the United Kingdom and subsequently validated in multiple health system contexts, demonstrated clinically meaningful improvements in pain, physical function, and quality of life in patients with chronic knee and hip pain from osteoarthritis, with effect sizes comparable to those achieved by non-steroidal anti-inflammatory drugs and significantly superior to passive treatments including electrotherapy and acupuncture. Critically, these improvements were achieved without accelerating joint damage on serial imaging — the fear that exercise harms arthritic joints is not supported by the radiographic evidence.
Aerobic exercise programs — walking, cycling, hydrotherapy, and Tai Chi — have demonstrated consistent benefits for pain reduction and functional improvement across a range of osteoarthritis populations, including older adults, those with significant obesity, and those with moderate-to-severe radiographic disease. The hydrotherapy environment deserves specific mention: the buoyancy of water reduces effective body weight by approximately sixty percent at chest depth, allowing patients with severe load-related knee pain to perform aerobic exercise and range-of-motion activities that they cannot comfortably achieve on land, while the hydrostatic pressure of immersion provides additional support to swollen periarticular soft tissues.
Mind-body exercise modalities, particularly Tai Chi, have accumulated a robust evidence base in knee osteoarthritis over the past two decades. A landmark trial published in the Annals of Internal Medicine demonstrated that Tai Chi was equivalent to physical therapy for improvement in pain, function, and quality of life at twelve-week and fifty-two-week follow-up in patients with symptomatic knee osteoarthritis, with additional benefits for depression scores and self-efficacy that conventional strength training programs did not demonstrate. This finding is clinically important because depression and low self-efficacy are among the strongest predictors of poor treatment adherence and functional decline in chronic musculoskeletal pain conditions — addressing them through the exercise intervention itself, rather than requiring separate psychological support, has practical therapeutic advantages.
The ESCAPE-pain program — Enabling Self-management and Coping of Arthritic Pain through Exercise — a structured group rehabilitation program developed in the United Kingdom and subsequently validated in multiple health system contexts, demonstrated clinically meaningful improvements in pain, physical function, and quality of life in patients with chronic knee and hip pain from osteoarthritis, with effect sizes comparable to those achieved by non-steroidal anti-inflammatory drugs and significantly superior to passive treatments including electrotherapy and acupuncture. Critically, these improvements were achieved without accelerating joint damage on serial imaging — the fear that exercise harms arthritic joints is not supported by the radiographic evidence.
Aerobic exercise programs — walking, cycling, hydrotherapy, and Tai Chi — have demonstrated consistent benefits for pain reduction and functional improvement across a range of osteoarthritis populations, including older adults, those with significant obesity, and those with moderate-to-severe radiographic disease. The hydrotherapy environment deserves specific mention: the buoyancy of water reduces effective body weight by approximately sixty percent at chest depth, allowing patients with severe load-related knee pain to perform aerobic exercise and range-of-motion activities that they cannot comfortably achieve on land, while the hydrostatic pressure of immersion provides additional support to swollen periarticular soft tissues.
Mind-body exercise modalities, particularly Tai Chi, have accumulated a robust evidence base in knee osteoarthritis over the past two decades. A landmark trial published in the Annals of Internal Medicine demonstrated that Tai Chi was equivalent to physical therapy for improvement in pain, function, and quality of life at twelve-week and fifty-two-week follow-up in patients with symptomatic knee osteoarthritis, with additional benefits for depression scores and self-efficacy that conventional strength training programs did not demonstrate. This finding is clinically important because depression and low self-efficacy are among the strongest predictors of poor treatment adherence and functional decline in chronic musculoskeletal pain conditions — addressing them through the exercise intervention itself, rather than requiring separate psychological support, has practical therapeutic advantages.
Breaking the Vicious Cycle: Pain, Fear, Avoidance, and Deconditioning
Understanding why so many patients with osteoarthritis remain physically inactive despite the evidence for exercise requires understanding the pain-fear-avoidance cycle that governs behavior in chronic musculoskeletal conditions. The cycle begins with the experience of pain during or after physical activity — a near-universal experience in active osteoarthritis patients that the nervous system, shaped by its evolutionary mandate to protect the organism from tissue damage, correctly identifies as a signal worthy of behavioral modification. The organism responds by reducing the activity that produced the pain, which provides short-term relief and reinforces the avoidance behavior.
Over weeks to months, this avoidance produces physical deconditioning: quadriceps atrophy, reduced cardiovascular fitness, increased body weight, and the progressive loss of the neuromuscular coordination and balance that protects the arthritic joint from injurious loading. The deconditioned joint is more painful than the conditioned one — because the muscular shock-absorbers have atrophied, because synovial fluid quality has declined from insufficient mechanical stimulation, and because the central sensitization that often accompanies chronic pain conditions has lowered the threshold at which nociceptive signals are perceived as painful. The deconditioned patient avoids more activity, deconditions further, and experiences more pain — a self-perpetuating spiral that leads, in many cases, toward surgical consultation for joint replacement.
Effective exercise therapy for osteoarthritis must therefore address not only the physical deconditioning but the cognitive and psychological dimensions of the pain-fear-avoidance cycle. Pain education — teaching patients that pain during exercise in osteoarthritis does not indicate tissue damage, that the joint can tolerate graduated loading, and that the discomfort experienced during the early stages of an exercise program represents normal physiological adaptation rather than injury — is as important as the exercise prescription itself. Patients who understand the biology of their pain, who have a conceptual model of why movement helps rather than harms, are significantly more likely to adhere to exercise programs and to sustain the functional gains they produce.
Over weeks to months, this avoidance produces physical deconditioning: quadriceps atrophy, reduced cardiovascular fitness, increased body weight, and the progressive loss of the neuromuscular coordination and balance that protects the arthritic joint from injurious loading. The deconditioned joint is more painful than the conditioned one — because the muscular shock-absorbers have atrophied, because synovial fluid quality has declined from insufficient mechanical stimulation, and because the central sensitization that often accompanies chronic pain conditions has lowered the threshold at which nociceptive signals are perceived as painful. The deconditioned patient avoids more activity, deconditions further, and experiences more pain — a self-perpetuating spiral that leads, in many cases, toward surgical consultation for joint replacement.
Effective exercise therapy for osteoarthritis must therefore address not only the physical deconditioning but the cognitive and psychological dimensions of the pain-fear-avoidance cycle. Pain education — teaching patients that pain during exercise in osteoarthritis does not indicate tissue damage, that the joint can tolerate graduated loading, and that the discomfort experienced during the early stages of an exercise program represents normal physiological adaptation rather than injury — is as important as the exercise prescription itself. Patients who understand the biology of their pain, who have a conceptual model of why movement helps rather than harms, are significantly more likely to adhere to exercise programs and to sustain the functional gains they produce.
Exercise Prescription: What Type, How Much, and How to Start Aerobic Exercise: Building the Foundation
Current guidelines recommend that patients with knee or hip osteoarthritis engage in at least 150 minutes per week of moderate-intensity aerobic exercise — consistent with the general population physical activity recommendations of major health organizations globally. For patients who are significantly deconditioned, this target should be approached gradually: starting with ten to fifteen minutes of low-intensity walking or cycling on alternate days, and increasing duration by no more than ten percent per week to allow musculoskeletal adaptation without overloading.
Walking remains the most accessible and most widely studied aerobic modality for osteoarthritis. The Nordic walking variant — using poles to distribute upper-body loading and reduce knee joint contact forces during the gait cycle — has shown particular benefit in patients with moderate-to-severe knee pain, allowing a longer stride length and greater exercise intensity without the pain increment that unsupported walking at the same speed would produce. Cycling — both outdoor and stationary — is an excellent alternative or supplement to walking, offering the cardiovascular and quadriceps-strengthening benefits of aerobic exercise with substantially lower tibiofemoral joint contact forces than walking.
Walking remains the most accessible and most widely studied aerobic modality for osteoarthritis. The Nordic walking variant — using poles to distribute upper-body loading and reduce knee joint contact forces during the gait cycle — has shown particular benefit in patients with moderate-to-severe knee pain, allowing a longer stride length and greater exercise intensity without the pain increment that unsupported walking at the same speed would produce. Cycling — both outdoor and stationary — is an excellent alternative or supplement to walking, offering the cardiovascular and quadriceps-strengthening benefits of aerobic exercise with substantially lower tibiofemoral joint contact forces than walking.
Resistance Training: The Core of Joint Protection
Resistance training targeting the periarticular musculature of the affected joint should be the centerpiece of any osteoarthritis exercise prescription. For knee osteoarthritis, the core exercises are quadriceps strengthening — through exercises including seated knee extension, straight-leg raises, wall slides, and terminal knee extension — combined with hip abductor and hip extensor strengthening, which reduces the valgus knee moment during gait that increases medial tibiofemoral compartment loading. Programs should begin with low-resistance, high-repetition sets and progress over six to eight weeks to higher resistance with lower repetitions, following the principles of progressive overload that are standard in evidence-based resistance training.
The timing of soreness after resistance training — delayed-onset muscle soreness peaking twenty-four to forty-eight hours after exercise — should be distinguished clearly from articular pain, and patients should be counseled that muscle soreness represents normal adaptive remodeling of the exercised tissue rather than joint damage. A useful clinical rule is that exercise-related pain should return to baseline within twenty-four hours of completing the session; if pain remains elevated beyond this window, the exercise load should be reduced in the subsequent session and increased more gradually thereafter.
The timing of soreness after resistance training — delayed-onset muscle soreness peaking twenty-four to forty-eight hours after exercise — should be distinguished clearly from articular pain, and patients should be counseled that muscle soreness represents normal adaptive remodeling of the exercised tissue rather than joint damage. A useful clinical rule is that exercise-related pain should return to baseline within twenty-four hours of completing the session; if pain remains elevated beyond this window, the exercise load should be reduced in the subsequent session and increased more gradually thereafter.
Neuromuscular and Balance Training: Restoring Arthrogenic Inhibition
Neuromuscular training — exercises that challenge proprioception, dynamic balance, and the coordinated activation of periarticular muscle groups during functional movement — addresses the arthrogenic muscle inhibition that conventional resistance training may not fully reverse. Exercises including single-leg stance with perturbation, step-up and step-down tasks with trunk control challenges, and functional movement patterns such as sit-to-stand practice under progressive loading conditions have demonstrated benefits for knee proprioception, functional balance, and fall risk reduction in osteoarthritis populations. These exercises are particularly important for patients with a history of falls, those with significant quadriceps inhibition on clinical examination, and those with bilateral lower limb involvement.
Weight Management: The Compounding Benefit of Exercise Beyond the Joint
The relationship between body weight and knee osteoarthritis is biomechanically straightforward: for every kilogram of body weight, the tibiofemoral joint experiences approximately three to five kilograms of compressive force during level walking, and higher multiples during stair climbing and rising from a chair. A five-kilogram reduction in body weight therefore reduces knee joint loading by fifteen to twenty-five kilograms per step — a biomechanical dividend that compounds across thousands of steps per day and accumulates across years of sustained weight management.
The ADAPT trial — Arthritis, Diet, and Activity Promotion Trial — demonstrated that the combination of dietary weight loss and exercise produced greater improvements in knee pain, function, and mobility than either intervention alone, and that the combined intervention achieved its benefits through both the mechanical unloading of weight reduction and the direct biological effects of exercise described above. The synergy between these two components of the prescription is not merely additive — it is multiplicative, because the improved mobility produced by exercise enables the sustained physical activity that sustains weight management, and the reduced joint loading of weight loss enables the exercise intensity required for meaningful musculoskeletal conditioning.
Beyond its biomechanical benefits, adipose tissue reduction in patients with obesity-associated osteoarthritis reduces the systemic inflammatory burden that drives chondrocyte catabolism. Adipose tissue — particularly visceral adipose tissue — is a metabolically active endocrine organ that secretes adipokines including leptin, adiponectin, resistin, and visfatin, several of which have been identified as direct stimulators of pro-inflammatory cytokine production and cartilage matrix degradation in osteoarthritis. This metabolic-inflammatory pathway helps explain why osteoarthritis is prevalent in non-weight-bearing joints such as the hands and wrists of obese patients, and why the benefits of weight loss for osteoarthritis extend beyond simple mechanical unloading.
The ADAPT trial — Arthritis, Diet, and Activity Promotion Trial — demonstrated that the combination of dietary weight loss and exercise produced greater improvements in knee pain, function, and mobility than either intervention alone, and that the combined intervention achieved its benefits through both the mechanical unloading of weight reduction and the direct biological effects of exercise described above. The synergy between these two components of the prescription is not merely additive — it is multiplicative, because the improved mobility produced by exercise enables the sustained physical activity that sustains weight management, and the reduced joint loading of weight loss enables the exercise intensity required for meaningful musculoskeletal conditioning.
Beyond its biomechanical benefits, adipose tissue reduction in patients with obesity-associated osteoarthritis reduces the systemic inflammatory burden that drives chondrocyte catabolism. Adipose tissue — particularly visceral adipose tissue — is a metabolically active endocrine organ that secretes adipokines including leptin, adiponectin, resistin, and visfatin, several of which have been identified as direct stimulators of pro-inflammatory cytokine production and cartilage matrix degradation in osteoarthritis. This metabolic-inflammatory pathway helps explain why osteoarthritis is prevalent in non-weight-bearing joints such as the hands and wrists of obese patients, and why the benefits of weight loss for osteoarthritis extend beyond simple mechanical unloading.
When Exercise and Surgery Intersect: The Role of Prehabilitation and Postoperative Rehabilitation
For patients with advanced osteoarthritis who proceed to total joint replacement — the surgical option for end-stage disease that, when appropriate and well-timed, produces durable and substantial improvements in pain and function — exercise remains critically important on both sides of the operating table. Prehabilitation — structured preoperative exercise targeting quadriceps strength, cardiovascular fitness, and functional mobility — has been shown in randomized trials to reduce postoperative length of stay, reduce the need for inpatient rehabilitation, and improve functional outcomes at six and twelve months following total knee arthroplasty. The patient who arrives at surgery with stronger muscles and better cardiovascular fitness recovers faster, requires fewer postoperative analgesics, and achieves superior functional outcomes than the patient who arrives deconditioned.
Postoperative rehabilitation following total joint replacement is not supplementary care — it is the mechanism by which the surgical intervention is converted into functional improvement. A well-implanted prosthesis in a patient whose neuromuscular control has not been restored through rehabilitation will underperform compared to the same prosthesis in a patient who has completed an adequate rehabilitation program. The transition from the immediate postoperative period through progressive weight-bearing, range-of-motion restoration, strength training, and ultimately return to full functional activity follows the same biological principles as the exercise prescription for non-operative osteoarthritis management — it simply does so in the context of a surgically altered joint architecture.
Postoperative rehabilitation following total joint replacement is not supplementary care — it is the mechanism by which the surgical intervention is converted into functional improvement. A well-implanted prosthesis in a patient whose neuromuscular control has not been restored through rehabilitation will underperform compared to the same prosthesis in a patient who has completed an adequate rehabilitation program. The transition from the immediate postoperative period through progressive weight-bearing, range-of-motion restoration, strength training, and ultimately return to full functional activity follows the same biological principles as the exercise prescription for non-operative osteoarthritis management — it simply does so in the context of a surgically altered joint architecture.
Conclusion: Move More, Not Less — and Start Today
The person in the opening image — seated, still, hands wrapped around a painful knee — is not doing anything wrong. They are responding to pain in the most natural way that pain permits. But the evidence is unambiguous: that position, sustained over days and weeks and months, is the position in which osteoarthritis worsens. The synovial fluid stagnates. The chondrocytes starve. The quadriceps atrophies. The joint loads less tolerantly with each successive episode of guarded ambulation. The couch, in the long run, is not a refuge from osteoarthritis. It is one of its most reliable accomplices.
The gym — or the pool, or the cycling path, or the physiotherapy gym, or the living room floor with a resistance band — is where that trajectory is reversed. Not because exercise is painless, particularly at the beginning. Not because it is easy for someone who has been avoiding movement for months or years to re-engage with physical loading. But because the biology of the arthritic joint is responsive to the right mechanical inputs, and because the evidence that structured exercise reduces pain, improves function, slows disease progression, and reduces the likelihood of surgical intervention is more robust than the evidence for any pharmacological agent currently available for osteoarthritis.
Motion, as the evidence conclusively demonstrates, is indeed lotion — and the prescription is free, available immediately, and the most powerful tool in the management of osteoarthritis that medicine currently possesses. The role of the clinician is to prescribe it with the same specificity, confidence, and follow-up that they would apply to any other evidence-based treatment — and to help patients understand not just what to do, but why their joints need it.
The gym — or the pool, or the cycling path, or the physiotherapy gym, or the living room floor with a resistance band — is where that trajectory is reversed. Not because exercise is painless, particularly at the beginning. Not because it is easy for someone who has been avoiding movement for months or years to re-engage with physical loading. But because the biology of the arthritic joint is responsive to the right mechanical inputs, and because the evidence that structured exercise reduces pain, improves function, slows disease progression, and reduces the likelihood of surgical intervention is more robust than the evidence for any pharmacological agent currently available for osteoarthritis.
Motion, as the evidence conclusively demonstrates, is indeed lotion — and the prescription is free, available immediately, and the most powerful tool in the management of osteoarthritis that medicine currently possesses. The role of the clinician is to prescribe it with the same specificity, confidence, and follow-up that they would apply to any other evidence-based treatment — and to help patients understand not just what to do, but why their joints need it.