-
-
-
Jakarta, Indonesia
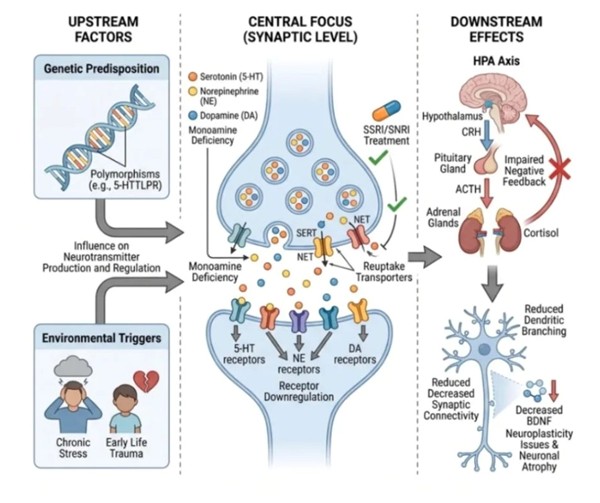
The Silent Atrophy: Why We Are Rewriting Rules on Major Depressive Disorders?

The Critical Impact of Delayed Varicocelectomy on Testicular Atrophy
Understanding Varicocele and the Race Against Time
A varicocele is an abnormal enlargement of the pampiniform venous plexus — the network of veins that drains blood from the testis. In a healthy testis, this drainage system operates efficiently, maintaining the slightly cooler-than-body temperature that is essential for optimal sperm production and testicular function. When a varicocele develops, however, the veins become dilated and dysfunctional, and blood begins to pool rather than drain freely. While not every varicocele demands immediate intervention, the central message of contemporary urology is unambiguous: time is not neutral in this condition. The longer a significant varicocele is left untreated, the greater the cumulative biological damage inflicted on the testis — damage that, in many cases, can become irreversible. Recognizing this window of opportunity, and acting within it, is the cornerstone of preserving male reproductive health.
The Healthy Testis: An Environment Built for Precision
In its early or untreated stage, a testis with a clinically insignificant varicocele — or no varicocele at all — functions within a carefully regulated environment. Blood flows efficiently through the pampiniform plexus, carrying away metabolic waste products and delivering oxygen-rich supply to the testicular tissue. The scrotal anatomy itself plays a role in this regulation: by positioning the testes outside the body cavity, nature ensures they remain approximately 2–4 degrees Celsius cooler than core body temperature, a condition that is absolutely necessary for normal spermatogenesis. Within this optimal environment, the germinal epithelium of the testis thrives, producing sperm of high motility, normal morphology, and robust DNA integrity. The consequence is high sperm quality — a biological asset that, under normal circumstances, is reliably maintained throughout a man's reproductive years.
Venous Reflux and the Cascade of Damage
As a varicocele progresses and treatment is delayed, the consequences are not static — they are cumulative and self-reinforcing. Venous reflux, the backward flow of blood through incompetent valves in the spermatic vein, drives warm, deoxygenated blood into the pampiniform plexus. This produces two simultaneous and interacting forms of physiological injury. First, blood pooling causes a sustained elevation in scrotal temperature, exposing the testis to a thermal environment it was never designed to tolerate. Second, the resulting oxidative stress — an imbalance between harmful reactive oxygen species and the testis's antioxidant defenses — begins to damage sperm DNA, impair the function of Leydig cells responsible for testosterone production, and compromise the Sertoli cells that nurture developing sperm. Together, these insults create a biochemical environment that is actively hostile to spermatogenesis, and the damage accrues with every month that intervention is deferred.
Testicular Atrophy: The Visible Toll of Delayed Treatment
One of the most clinically significant consequences of a long-standing, untreated varicocele is testicular atrophy — a measurable reduction in testicular volume. This shrinkage is not merely cosmetic; it is a direct indicator of the underlying loss of functional testicular parenchyma. As the germinal epithelium deteriorates under the combined assault of heat and oxidative damage, the structural integrity of the testis diminishes. Progressive volume loss can be tracked sonographically, and studies have consistently demonstrated that the degree of atrophy correlates with both the duration of the varicocele and the severity of its hemodynamic effects. In adolescents and young men — who are at a critical developmental window — the impact of atrophy is particularly profound, as the affected testis may fail to achieve its expected growth trajectory, setting the stage for long-term reproductive compromise.
Fertility at Stake: The Sperm Quality Consequence
The downstream impact of all this testicular damage ultimately converges on a single, deeply consequential outcome: reduced fertility potential. Sperm produced in a testis subjected to chronic thermal and oxidative stress are measurably inferior — diminished in count, impaired in motility, abnormal in morphology, and frequently carrying elevated levels of DNA fragmentation. This deterioration in sperm quality is not an abstract laboratory finding; it translates directly into lower rates of natural conception and poorer outcomes with assisted reproductive technologies. The contrast with the healthy testis could not be starker: where optimal conditions yield high sperm quality and robust fertility, the delayed varicocele creates a slow and silent fertility crisis. Varicocelectomy, when performed in a timely manner, has been demonstrated in numerous studies to reverse or significantly improve these parameters — underscoring that the surgical decision is, in many cases, a decision for or against a man's reproductive future.
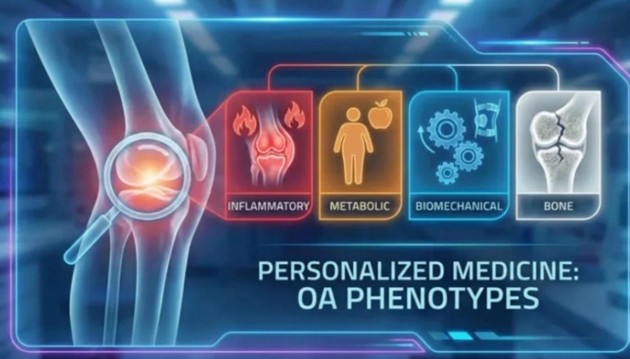
Motion is Lotion: Why the Gym is the Unexpected Best Friend of Your Osteoarthritis
Reframing physical activity from a feared aggravator to the most evidence-based, non-surgical intervention available for joint pain, stiffness, and functional decline in osteoarthritis