-
-
-
Jakarta, Indonesia
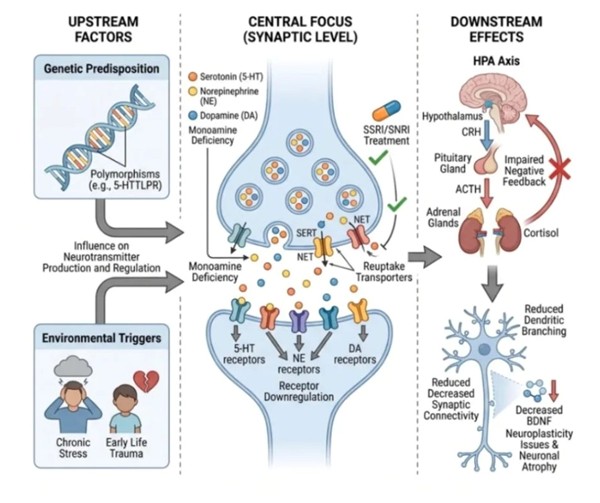
The Silent Atrophy: Why We Are Rewriting Rules on Major Depressive Disorders?

The Evolution of RSI: Why "No Ventilation" is No Longer the Rule
The Classic Dogma: Why "Do Not Ventilate" Became Law
For decades, the gold standard in emergency airway management held a rule so absolute it was printed in textbooks and drilled into generations of emergency physicians, anesthesiologists, and intensivists without qualification: during Rapid Sequence Induction, you do not ventilate the patient. The rationale behind this doctrine was physiologically sound in its original context — RSI was designed for patients at high risk of pulmonary aspiration, particularly those with a full stomach, and mask ventilation between drug administration and laryngoscopy was believed to insufflate gas into the stomach, raising intragastric pressure and increasing the risk of regurgitation of gastric contents into an unprotected airway. The sequential combination of a rapidly acting induction agent and a depolarizing neuromuscular blocking agent — classically succinylcholine — was intended to produce unconsciousness and complete paralysis within 60 seconds, at which point the clinician would intubate without ever having delivered a breath. This rigid no-ventilation interval was not a suggestion; it was the standard of care, institutionally reinforced and rarely questioned for nearly half a century.
The Turning Point: When Evidence Challenged the Rule
The shift in practice did not happen overnight, nor was it born from theoretical debate alone. It was driven by accumulating evidence from emergency departments and critical care units worldwide revealing an uncomfortable truth: patients undergoing classic RSI — particularly those who were already hypoxic from respiratory failure, sepsis, or trauma — were experiencing critical desaturation events during the apneic interval that, in some cases, were causing severe harm or death. Critically ill patients have markedly reduced oxygen reserves compared to elective surgical patients, and the 60 to 90 seconds of apnea inherent in the classic technique was, for many of them, dangerously long. Simultaneously, the evidence base supporting the aspiration risk of gentle bag-mask ventilation proved far weaker than historical doctrine had implied. Studies demonstrated that properly applied low-pressure ventilation with attention to cricoid pressure produced minimal gastric insufflation. The medical community was forced to confront a difficult reality: the rule designed to prevent one catastrophic complication was, in certain high-risk populations, precipitating another. Progress demanded a more nuanced, patient-centered approach.
The Modern Approach: Gentle Ventilation and Apneic Oxygenation
The Modified RSI that has emerged from this evidence revolution is not an abandonment of safety — it is a recalibration of where the risk actually lies for each individual patient. The two cornerstones of this modern approach are gentle ventilation and apneic oxygenation, and together they address the most dangerous phase of the intubation sequence with a specificity that the blunt rule of the past could never provide. Gentle ventilation — defined as low-pressure, low-tidal-volume bag-mask breaths delivered after induction and paralysis — serves to pre-oxygenate and maintain oxygen saturation during a prolonged apneic phase, particularly in patients who desaturate rapidly. The emphasis on "gentle" is deliberate: low inflation pressures below 20 cmH₂O minimize the risk of gastric insufflation that the classic doctrine sought to avoid, preserving the safety rationale while eliminating the physiological penalty of uncorrected hypoxia. Apneic oxygenation, the second pillar, exploits a well-established physiological phenomenon: even in an apneic, paralyzed patient, passive high-flow oxygen delivered via nasal cannula at 15 liters per minute continues to diffuse down a concentration gradient from the nasopharynx into the alveoli through a process called diffusion oxygenation. Clinical trials, including landmark studies from emergency departments managing critically ill patients, have demonstrated that apneic oxygenation can extend the safe apneic period by several minutes, dramatically reducing the incidence of critical desaturation events. For the modern emergency physician, Modified RSI is not a compromise — it is the evidence-based synthesis of decades of clinical learning.
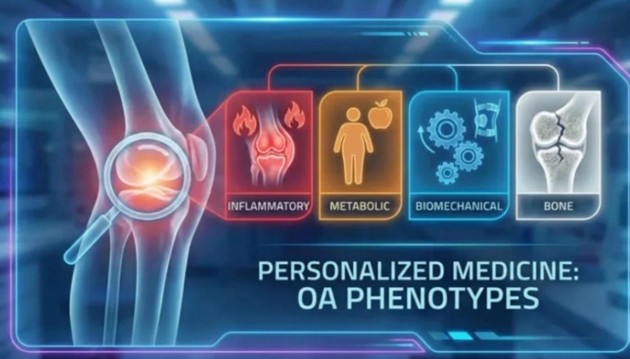
Motion is Lotion: Why the Gym is the Unexpected Best Friend of Your Osteoarthritis
Reframing physical activity from a feared aggravator to the most evidence-based, non-surgical intervention available for joint pain, stiffness, and functional decline in osteoarthritis