-
-
-
Jakarta, Indonesia
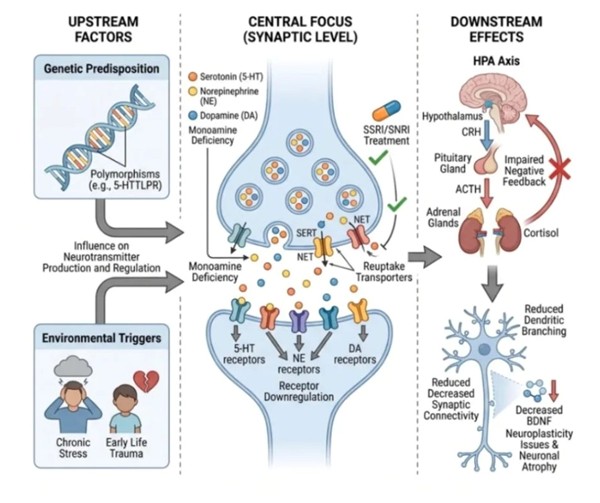
The Silent Atrophy: Why We Are Rewriting Rules on Major Depressive Disorders?

PCOS: Understanding and Actively Managing Polycystic Ovary Syndrome — A Holistic Guide
The Interconnected Cycle: Why PCOS Is More Than a Reproductive Condition
Polycystic Ovary Syndrome is frequently mischaracterized as simply a problem with the ovaries, but this framing fundamentally understates the condition's complexity. PCOS is, at its core, a systemic endocrine and metabolic disorder in which the ovaries, insulin regulation, and hormonal pathways are locked in a continuous, self-reinforcing cycle of dysfunction. In many women with PCOS, the root driver is insulin resistance — a state in which the body's cells fail to respond normally to insulin, prompting the pancreas to produce ever-higher levels of it. Elevated insulin, in turn, signals the ovaries to overproduce androgens — male-type hormones — which then disrupt normal follicular development and prevent regular ovulation. The resulting hormonal imbalance feeds back into worsening insulin resistance, completing a loop that perpetuates itself unless deliberately interrupted. Understanding this cycle is not merely academic; it is the essential first step toward choosing interventions that address the actual biological drivers rather than simply masking symptoms.
Nutrition as Medicine: The Power of the Anti-Inflammatory Plate
Among the lifestyle interventions available to women with PCOS, dietary modification stands as one of the most impactful and accessible. The central nutritional goal in PCOS management is stabilizing blood glucose and, by extension, insulin levels — and this is best achieved through a low-glycemic, anti-inflammatory eating pattern. Foods rich in fiber, healthy fats, lean proteins, and antioxidants — such as berries, nuts, legumes, leafy greens, and fatty fish — help blunt post-meal glucose spikes and reduce the chronic, low-grade inflammation that many women with PCOS experience. Conversely, highly processed carbohydrates, refined sugars, and inflammatory seed oils can exacerbate insulin resistance and worsen androgenic symptoms. Research consistently demonstrates that even modest dietary improvements, without significant caloric restriction, can meaningfully improve hormonal profiles, restore menstrual regularity, and support fertility — making the daily composition of meals a genuine therapeutic tool in PCOS care.
Movement and Supplementation: Building the Metabolic Foundation
Physical activity is one of the most potent natural tools for improving insulin sensitivity — the very mechanism that underpins much of PCOS pathophysiology. Regular movement, even at the level of a brisk 8,000-step daily walk, activates glucose transporters in muscle cells and reduces dependence on insulin for glucose uptake, effectively giving the pancreas relief from chronic overproduction. Both aerobic exercise and resistance training have demonstrated benefits in PCOS, with studies showing improvements in fasting insulin levels, testosterone concentrations, menstrual cycle regularity, and body composition. Alongside physical activity, targeted supplementation plays a complementary role. Vitamin D deficiency is disproportionately prevalent among women with PCOS and is associated with worse insulin resistance, greater androgenic activity, and lower fertility. Correcting this deficiency through supplementation has shown promising effects on hormonal balance and metabolic markers. Inositol compounds, particularly myo-inositol and D-chiro-inositol, have also emerged as evidence-backed supplements that can improve ovarian function and insulin signaling. Together, movement and smart supplementation form a metabolic foundation upon which all other PCOS management efforts can build more effectively.
The Journal as a Tool: Owning Your PCOS Journey
PCOS is one of the most heterogeneous conditions in women's health — no two patients present identically, and the relative contribution of hormonal versus metabolic versus inflammatory factors varies considerably between individuals. This reality makes self-tracking not just a motivational exercise but a clinically meaningful practice. Keeping a dedicated symptom and lifestyle journal allows a woman to identify which dietary choices affect her energy and bloating, which exercise patterns seem to correlate with improved cycle regularity, and which stressors reliably trigger symptom flares. Over time, this personalized data becomes invaluable — both for the patient herself and for her healthcare team, enabling treatment plans to be adjusted with precision rather than guesswork. Tracking menstrual cycle data, whether through a notebook or a dedicated app, also provides an objective measure of treatment response, helping to distinguish genuine progress from normal cycle-to-cycle variation. In a condition as individual as PCOS, the patient who understands her own patterns is the most empowered partner in her own care.
Motion is Lotion: Why the Gym is the Unexpected Best Friend of Your Osteoarthritis
Reframing physical activity from a feared aggravator to the most evidence-based, non-surgical intervention available for joint pain, stiffness, and functional decline in osteoarthritis